Building Back Better: Towards Advancing Global Healthy Security
2022 started with the largest increase in COVID-19 infections globally. Compared to the peaks of less than 900,000 new cases per day in the emergence of the “Delta Variant” in early 2021, the “Omicron Variant” reached a peak of more than 3.8 million new cases per day towards the end of January 2022, according to the Worldometer database. As of mid-February, there have been more than 410 million COVID-19 cases, and more than 5.8 million deaths.
Vaccine Success, But No Panacea
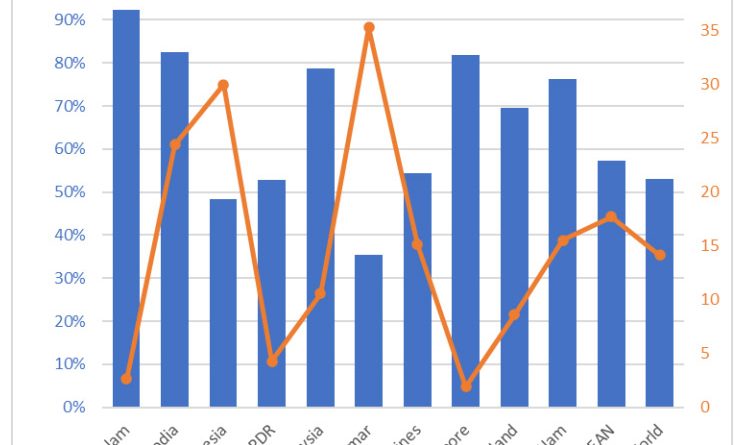
Vaccines have been seen as a key mechanism for addressing the pandemic. Data from the World Health Organization (WHO) show that as of mid-February, 4.8 billion individuals (60.7%) have received at least one dose of a COVID-19 vaccine, of which 4.2 billion are fully inoculated (53%). The ASEAN region showed moderate success. Across its population of 667 million individuals, 458 million individuals (69%) have received at least one dose, of which 382 million individuals (57%) are fully inoculated—which are better than the global average.
However, just because the average vaccination levels in ASEAN are higher than the global average, it does not mean that ASEAN has been doing better than the rest of the world in preventing deaths. In fact, ASEAN is doing worse in keeping the case fatality rate low: whereas the world average is 14 deaths for every 1,000 cases, ASEAN has an average of 17 deaths per 1,000 cases.
This is not to say that vaccines have not been effective. However, vaccines are no panacea for dealing with the kinds of health security challenges facing the world today. The on-going pandemic has shown that more lessons are to be learnt and much more should be done to be able to ‘build back better’ and advance global health security.
Dealing with Health Inequities
One of the ugly realities that the COVID-19 pandemic has revealed is vaccine inequity. At the height of the health crisis, many high-income countries (HICs) and wealthy economies had signed exclusive bilateral agreements with vaccine manufacturers to ensure enough doses for their citizens causing severe problems of vaccine access for less developed countries. And despite calls from the WHO for HICs to help ease supply constraints and increase their donations to COVAX facility to help countries in need, many HICs have instead shifted their focus toward giving booster doses to give their citizens more protection against new variants of the virus like Delta and Omicron.
Against these challenges, the Pandemic Treaty has been advanced to make countries more accountable to one another. A key agenda is to support the waiving of intellectual property and promote technology and knowledge transfer to allow production in countries that have the capacity to manufacture vaccines and other therapeutics for COVID-19 and other emerging pandemics.
Another important agenda is to strengthen health systems from the local, national to regional levels in order to ‘build back better’. This requires significant investments of resources, including training the healthcare workforce in the region, greater cooperation in ramping up scientific and medical expertise, and providing resources to build capacity of laboratories and public health facilities.
Last, but certainly not least, is the need to increase protection for more vulnerable groups, particularly those who are extremely poor, the elderly and those with disabilities who have no access to healthcare. Thus, a key priority for advancing global health security in a post-Covid world is to provide universal healthcare. This is certainly one way to build “shock-responsive” social protection systems to help people deal with threats to health and other human security problems.